
HBF Blog
From real member stories to trusted investigations into different cover options, we’ve carefully curated these articles to help you get the best cover for your health and the things that matter to you.

Meet your health savvy self
We’re setting you up with the research, resources, and really important questions you need to navigate your health journey with confidence.
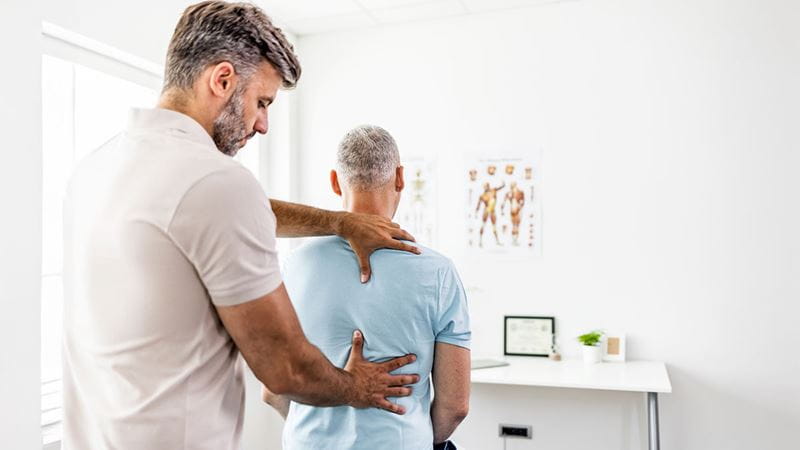
Early recovery after spinal fusion focuses on safe movement, gentle activity.
19 March 2026
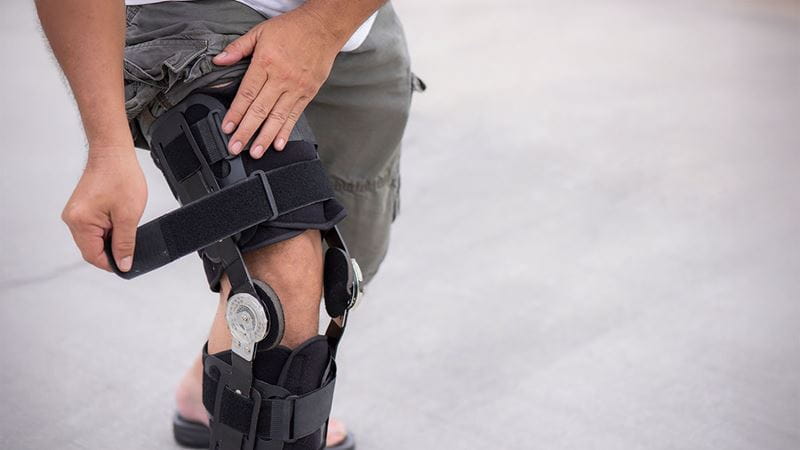
Early recovery after a knee replacement focuses on managing pain.
18 March 2026

Early recovery after a hip replacement focuses on managing pain.
18 March 2026

Early recovery after an ACL reconstruction focuses on restoring knee movement.
18 March 2026

Recovering from shoulder surgery can feel daunting.
17 March 2026

It’s officially HBF Run for a Reason season and if you’re lacing up for this year’s Brooks Half Marathon and wondering about shoes...
17 March 2026

The protein-in-everything trend has been centerstage for some time in the social media nutrition world.
16 March 2026

Due for a dentist visit? Booking a dental appointment isn’t just a tick for your teeth, it’s something your whole body can benefit from.
3 March 2026

Overtraining detection, hydration predictor, stress level monitoring…
24 February 2026

Year after year our socks are knocked off at the incredible families running.
9 February 2026

The start of the year brings grand plans and goals, and after a summer of social events and celebrations, drinking less may be the plan.
9 February 2026

Cross training isn’t just a buzzword, it’s a proven strategy for better running and a great mental refresh.
9 February 2026

You’ve got your training plan in motion, your diet dialled but have you thought about your mental preparation?
8 February 2026

Here’s a practical guide to meals and snacks for training days and race day, designed by CSIRO dietitians.
29 January 2026

What you eat can be the difference between feeling strong ... and hitting the wall.
28 January 2026